The spectrum of mental health: part 1 - full & partial syndrome disorders
Last updated on 23rd February 2011
This blog post is downloadable as both a Word doc & a PDF file.
Different degrees of "mental health": At any point in time, a proportion of people are suffering from some type of formally diagnosable mental disorder. Others are subsyndromal - struggling although not qualifying for the full criteria of any specific diagnosis. Some people are "doing OK" - they are in moderate mental health. And some are doing particularly well emotionally, cognitively, in relationships & in general functioning - they're really "flourishing".
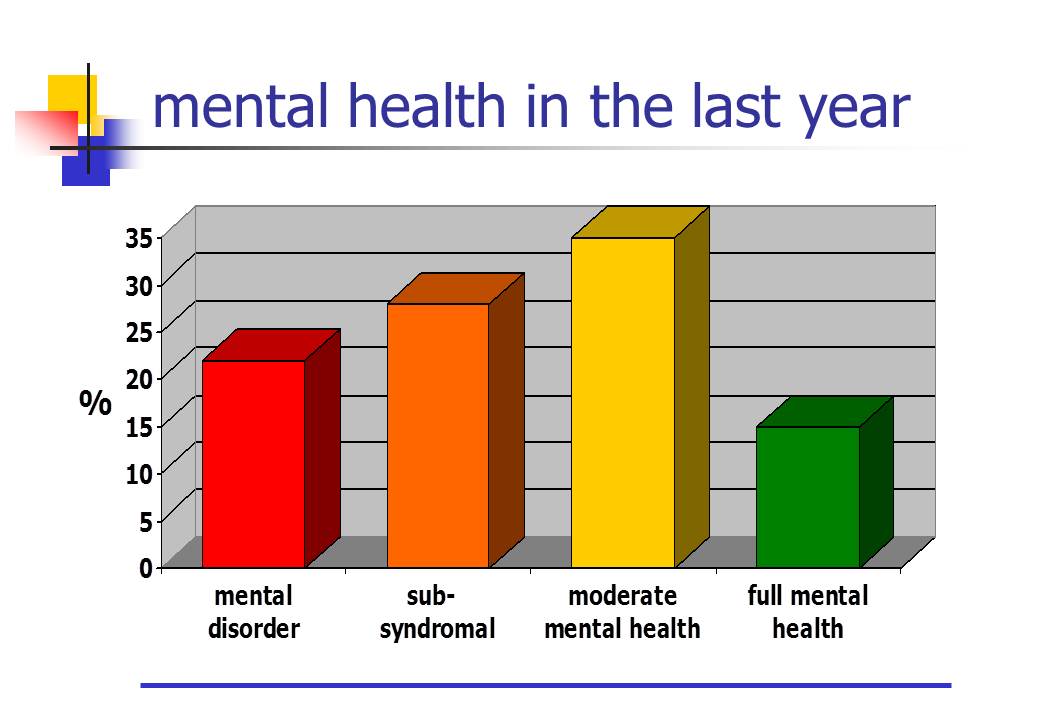
What proportion of the population is in each of these four states? As the diagram (above) illustrates, mental health is distributed as a spectrum across the population. The cut-off points between the four states are somewhat arbitrary, but overall the diagram highlights very important variations in levels of happiness, distress, & overall functioning. The prevalence of these four states will vary with the group being surveyed and the country in which the survey is being done. Typically though, in developed countries, each year about 20% or more of the adult population will suffer from a full syndrome mental or substance use disorder. A higher proportion will suffer a troublesome mix of mental symptoms causing significant distress & impairment, but not qualifying as a full clinical syndrome. 30 to 40% of the population can be classified as enjoying "moderate mental health", and less than 20% are flourishing with all the positive associated benefits for mood, resilience & functioning.
Mental disorder: A recent prospective investigation (Moffitt, Caspi et al. 2010) interviewing people on a series of occasions over a number of years has shown that the true lifetime frequency of mental disorders has been considerably underestimated (due to previously relying on interviews done on only one occasion). The researchers found that, by age 32, at least 49.5% of people had experienced some form of diagnosable anxiety disorder, 31.8% had suffered from alcohol dependence, and 41.4% from depression. These estimates are actually too low rather than too high. The population interviewed were only assessed between the ages of 18 and 32, so child/adolescent and mid-life/old age disorders weren't measured. Even over the 15 years studied, only four "previous year" samples were taken. Earlier research (Narrow, Rae et al. 2002) had shown that 20.9% of adults, aged 18 to 54, had experienced a mental or substance use disorder in the previous year that had significantly impacted their life. The evidence is clear - in any year, about 1 in 5 of us will suffer a clinically significant, formally diagnosable mental or substance use disorder. Over our life time the majority of us - more than 1 in 2 - will, at some stage, experience this level of difficulty.
Subsyndromal symptoms & languishing: Full syndrome mental disorders are worryingly common. However the picture is even more concerning than this. For any individual suffering from a diagnosable mental disorder, there are even more people struggling with symptoms that don't qualify as a "full clinical disorder". These subsyndromal problems still cause significant suffering, impact to a troublesome extent on functioning, and are associated with increased risk of slipping into a full syndrome disorder in the future. This picture of common, distressing and disabling subsyndromal symptoms has - for example - been reported for depression (Ayuso-Mateos, Nuevo et al. 2010), bipolar disorder (Marangell, Dennehy et al. 2009), panic disorder (Skapinakis, Lewis et al. 2010), obsessive-compulsive disorder (de Bruijn, Beun et al. 2010), post-traumatic stress disorder (Zlotnick, Franklin et al. 2002), and social anxiety disorder (Ruscio, Brown et al. 2008). In fact a recent paper in the British Journal of Psychiatry (Rai, Skapinakis et al. 2010) concluded that " In a representative sample of the UK population we found that common mental disorders ... and subthreshold psychiatric symptoms at baseline were both independently associated with new-onset functional disability and significant days lost from work at 18-month follow-up. Subthreshold symptoms contributed to almost half the aggregate burden of functional disability and over 32 million days lost from work in the year preceding the study. Leaving these symptoms unaccounted for in surveys may lead to gross underestimation of disability related to psychiatric morbidity."
Two key points about full & partial syndrome mental disorders: I would like to make two major points about full & subsyndromal psychiatric disorders. The first is that - in the last year - probably between a third to a half of us have suffered from periods of psychological distress or substance abuse that have caused significant suffering and impacted troublesomely on our functioning. So if you have sadly been one of these people, then do realise that you are one of very many. It's still crucial to work to improve your situation, but it may help a little to know you are not at all alone. People don't go about with a label around their neck saying "Suffering from significant psychological symptoms" so often we don't realise how tremendously common these difficulties are. The second major point is the importance of trying to improve even residual symptoms. This is for three reasons - life is better quality & more enjoyable without troublesome psychological distress. Furthermore we relate to others better, work more productively and generally function more enjoyably when we're free of even subsyndromal symptoms. Thirdly these partial syndromes are major risk factors for subsequent full syndromes (Nierenberg, Husain et al. 2010; Vittengl, Clark et al. 2010). Getting better is like putting out a bonfire. Moving from a full syndrome to only a partial syndrome psychological disorder certainly feels better. However - like leaving a bonfire smouldering rather than making sure it's completely out - partial syndromes are one of the strongest indicators of risk for developing a subsequent full syndrome. The bonfire can easily flare up again. Try to get rid of residual symptoms - one is then both in a better and also in a more stable psychological state.
